In continuation of my update on Victoza (liraglutide)
The U.S. Food and Drug Administration approved Victoza (liraglutide) injection for treatment of pediatric patients 10 years or older with type 2 diabetes. Victoza is the first non-insulin drug approved to treat type 2 diabetes in pediatric patients since metformin was approved for pediatric use in 2000. Victoza has been approved to treat adult patients with type 2 diabetes since 2010.
“The FDA encourages drugs to be made available to the widest number of patients possible when there is evidence of safety and efficacy,” said Lisa Yanoff, M.D, acting director of the Division of Metabolism and Endocrinology Products in the FDA’s Center for Drug Evaluation and Research. “Victoza has now been shown to improve blood sugar control in pediatric patients with type 2 diabetes. The expanded indication provides an additional treatment option at a time when an increasing number of children are being diagnosed with this disease.”
Type 2 diabetes is the most common form of diabetes, occurring when the pancreas cannot make enough insulin to keep blood sugar at normal levels. Although type 2 diabetes primarily occurs in patients over the age of 45, the prevalence rate among younger patients has been rising dramatically over the past couple of decades. The Diabetes Report Card published by the U.S. Centers for Disease Control and Prevention estimates that more than 5,000 new cases of type 2 diabetes are diagnosed each year among U.S. youth younger than age 20.
Victoza improves blood sugar levels by creating the same effects in the body as the glucagon-like peptide (GLP-1) receptor protein in the pancreas. GLP-1 is often found in insufficient levels in type 2 diabetes patients. Like GLP-1, Victoza slows digestion, prevents the liver from making too much glucose (a simple sugar), and helps the pancreas produce more insulin when needed. As noted on the label, Victoza is not a substitute for insulin and is not indicated for patients with type 1 diabetes or those with diabetic ketoacidosis, a condition associated with diabetes where the body breaks down fat too quickly because there is inadequate insulin or none at all. Victoza is also indicated to reduce the risk of major adverse cardiovascular events in adults with type 2 diabetes and established cardiovascular disease; however, its effect on major adverse cardiovascular events in pediatrics was not studied and it is not indicated for this use in children.
The efficacy and safety of Victoza for reducing blood sugar in patients with type 2 diabetes was studied in several placebo-controlled trials in adults and one placebo-controlled trial with 134 pediatric patients 10 years and older for more than 26 weeks. Approximately 64% of patients in the pediatric study had a reduction in their hemoglobin A1c (HbA1c) below 7% while on Victoza, compared to only 37% who achieved these results with the placebo. HbA1c is a blood test that is routinely performed to evaluate how well a patient’s diabetes is controlled, and a lower number indicates better control of the disease. These results occurred regardless of whether the patient also took insulin at the same time. Adult patients who took Victoza with insulin or other drugs that increase the amount of insulin the body makes (e.g., sulfonylurea) may have an increased risk of hypoglycemia (low blood sugar). Meanwhile, pediatric patients 10 years and older taking Victoza had a higher risk of hypoglycemia regardless of whether they took other therapies for diabetes.
The prescribing information for Victoza includes a Boxed Warning to advise health care professionals and patients about the increased risk of thyroid C-cell tumors. For this reason, patients who have had, or have family members who have ever had medullary thyroid carcinoma (MTC) should not use Victoza, nor should patients who have an endocrine system condition called multiple endocrine neoplasia syndrome type 2 (MEN 2). In addition, people who have a prior serious hypersensitivity reaction to Victoza or any of the product components should not use Victoza. Victoza also carries warnings about pancreatitis, Victoza pen sharing, hypoglycemia when used in conjunction with certain other drugs known to cause hypoglycemia including insulin and sulfonylurea, renal impairment or kidney failure, hypersensitivity and acute gallbladder disease. The most common side effects are nausea, diarrhea, vomiting, decreased appetite, indigestion and constipation.
https://en.wikipedia.org/wiki/Liraglutide

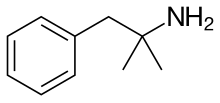 phentermine
phentermine 
 lorcaserin
lorcaserin Bupropion/naltrexone
Bupropion/naltrexone