In continuation of my update on Liraglutide

Dr. Ildiko Lingvay, Associate Professor of Internal Medicine and Clinical Sciences at UT Southwestern Medical Center, designed the clinical trial, which looked at the effectiveness of liraglutide in patients who were taking high doses of insulin.
"We have a growing population of obese patients who require larger and larger doses of insulin. The insulin causes them to put on more weight, which in turn means their glucose levels remain out of control. We wanted to test whether treating such patients with liraglutide would have an effect," said Dr. Lingvay.
Liraglutide, produced by Novo Nordisk, has several effects on the body: It increases insulin secretion; it reduces hunger; and it decreases glucagon secretion. Insulin and glucagon are molecules produced by the pancreas that have opposing effects, with insulin reducing blood sugar levels and glucagon increasing blood sugar levels. Insulin is secreted by beta cells in the pancreas and glucagon is secreted by alpha cells in the pancreas.
The study enrolled 71 Type 2 diabetes patients who were injecting large amounts of insulin each day, in most cases four or five shots a day. All of the patients had HbA1C levels that were 7.5 or higher (the goal for patients with diabetes is 7 or below). All of the patients were also overweight.
The patients in the study were randomly assigned to give themselves a daily injection of either a placebo or liraglutide in addition to their current therapy with a high dose of insulin. The results of the trial were clear, with the average HbA1C level of patients taking the drug dropping from 8.9 to 8, while long-term blood sugar levels were unchanged in the placebo group. The liraglutide patients also lost 4 ½ pounds on average, while the placebo group gained a small amount on average.
"This is less improvement than we normally see with liraglutide in patients who are not on insulin, but this is a huge improvement in a population that is so difficult to treat," said Dr. Lingvay.
Although the study was blinded - neither patients nor researchers knew which group a patient was assigned to - Ms. Sweat said that after a few weeks of being in the study she was sure that she had been assigned to the liraglutide group because her blood sugars were dropping dramatically.
"I thought I was doing the drug because my sugar finally went to normal," she said. "From the day I was diagnosed, my sugar was always high. After I started the study, for the first time in my life, my HbA1C went down, and I kept thinking, 'I must be taking the drug.' "
When the study ended, her physician prescribed liraglutide for her-whose attempt with other drugs were not successful."I give myself a shot every morning," the Garland woman said, adding that not only is her blood sugar level consistently better than it had been at any time before the study, but she has maintained a modest weight loss since the study began as well.
The study that Dr. Lingvay designed also looked at the mechanisms of action of liraglutide on this group of patients and the effect of the drug on the underlying disease, measuring insulin and glucagon blood levels following a meal.
The findings: Insulin production went up.
"The results were counterintuitive," said Dr. Lingvay. "One might expect that patients with such long-standing disease would have little or no residual beta-cell function and improvements would be driven through suppression of glucagon. To the contrary, we found that liraglutide exerted its hypoglycemic effect through improving insulin secretion."



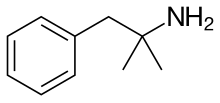 phentermine
phentermine 
 lorcaserin
lorcaserin Bupropion/naltrexone
Bupropion/naltrexone
