"We see great perspectives in the discovery because our data shows that the drug is effective against infections that occur because of what are known as Gram-negative bacteria. These bacteria form the basis of diseases such as pneumonia, cystitis and septic shock. Due to growing resistance, we are experiencing a decline in the number of effective treatments against them, and some of the medicaments which we otherwise know to be effective must be given in such high doses to be effective that they become toxic for the patients," explains Professor with special responsibilities (MSO) Thomas Vorup-Jensen from the Department of Biomedicine at Aarhus University.
Thursday, November 23, 2017
Multiple sclerosis drug can beat obstinate bacteria
Tuesday, January 28, 2020
AbbVie's HIV Drug Aluvia (Lopinavir/ritonavir) Seen as Potential Treatment for Coronavirus

Tuesday, November 10, 2015
Combatting viral and bacterial lung infections with volatile anesthetics: an interview with Dr Chakravarthy
Wednesday, May 25, 2011
Linezolid more effective than vancomycin in treating ventilated patients with MRSA pneumonia: Study
Linezolid more effective than vancomycin in treating ventilated patients with MRSA pneumonia: Study
Tuesday, March 3, 2020
FDA Approves Fetroja (cefiderocol) for the Treatment of Complicated Urinary Tract Infections

“Today’s approval provides an additional treatment option for patients with cUTIs who have limited or no alternative treatment options,” said John Farley, M.D., M.P.H., acting director of the Office of Infectious Diseases in the FDA’s Center for Drug Evaluation and Research. “A key global challenge the FDA faces as a public health agency is addressing the threat of antimicrobial-resistant infections, like cUTIs. This approval represents another step forward in the FDA’s overall efforts to ensure safe and effective antimicrobial drugs are available to patients for treating infections.”
Wednesday, September 7, 2016
FDA Approves Venclexta (venetoclax) for Chronic Lymphocytic Leukemia with 17p Deletion
In continuation of my update on Venclexta
Food and Drug Administration today approved Venclexta (venetoclax) for the treatment of patients with chronic lymphocytic leukemia (CLL) who have a chromosomal abnormality called 17p deletion and who have been treated with at least one prior therapy. Venclexta is the first FDA-approved treatment that targets the B-cell lymphoma 2 (BCL-2) protein, which supports cancer cell growth and is overexpressed in many patients with CLL.
Wednesday, April 22, 2015
Bitter gourd(Karela) leaves Medicinal uses
Phytochemical constituents of Bitter gourd Leaves
Medicinal Uses of Bitter gourd Leaves
- Drinking 10-15 ml juice of Karela leaves is beneficial in arthritis.
- Ascite (gastroenterological term for an accumulation of fluid in the peritoneal cavity)
- Extract 10-15 ml juice of leaves and add some honey and drink.
Monday, December 14, 2020
Fluvoxamine may prevent serious illness in COVID-19 patients, study suggests: Antidepressant drug repurposed for patients with coronavirus infection
The study, a collaboration between the university's Department of Psychiatry and Division of Infectious Diseases, involved 152 patients infected with SARS-CoV-2, the virus that causes COVID-19. Researchers compared the outcomes of those treated with fluvoxamine to the outcomes of those given an inactive placebo. After 15 days, none of the 80 patients who had received the drug experienced serious clinical deterioration. Meanwhile, six of the 72 patients given placebo (8.3%) became seriously ill, with four requiring hospitalization.
The study is published online Nov. 12 in the Journal of the American Medical Association.
"The patients who took fluvoxamine did not develop serious breathing difficulties or require hospitalization for problems with lung function," said the paper's first author, Eric J. Lenze, MD, the Wallace and Lucille Renard Professor of Psychiatry. "Most investigational treatments for COVID-19 have been aimed at the very sickest patients, but it's also important to find therapies that prevent patients from getting sick enough to require supplemental oxygen or to have to go to the hospital. Our study suggests fluvoxamine may help fill that niche."
Fluvoxamine is used commonly to treat obsessive-compulsive disorder (OCD), social anxiety disorder and depression. It is in a class of drugs known as selective serotonin-reuptake inhibitors (SSRIs), but unlike other SSRIs, fluvoxamine interacts strongly with a protein called the sigma-1 receptor. That receptor also helps regulate the body's inflammatory response.
"There are several ways this drug might work to help COVID-19 patients, but we think it most likely may be interacting with the sigma-1 receptor to reduce the production of inflammatory molecules," said senior author Angela M Reiersen, MD, an associate professor of psychiatry. "Past research has demonstrated that fluvoxamine can reduce inflammation in animal models of sepsis, and it may be doing something similar in our patients."
Reiersen said the drug's effects on inflammation could prevent the immune system from mounting an overwhelming response, which is thought to occur in some COVID-19 patients who seem to improve after a few days of illness and then worsen. Many of those patients end up hospitalized, and some die.
In an innovative twist to research during the pandemic, the study was conducted remotely. When a symptomatic patient tested positive and enrolled in the study, research staff delivered the medication or inactive placebo to them, along with thermometers, automatic blood pressure monitors and fingertip oxygen sensors.
"Our goal is to help patients who are initially well enough to be at home and to prevent them from getting sick enough to be hospitalized," said Caline Mattar, MD, an assistant professor of medicine in the Division of Infectious Diseases. "What we've seen so far suggests that fluvoxamine may be an important tool in achieving that goal."
For two weeks, subjects took either the antidepressant drug or placebo sugar pills while having daily interactions with members of the research team -- via phone or computer. That allowed patients to report on their symptoms, oxygen levels and other vital signs. If patients suffered shortness of breath or were hospitalized for pneumonia, or their oxygen saturation levels fell below 92%, their conditions were considered to have deteriorated.
"The good news is that not a single person taking the active medication experienced deterioration," Reiersen said. "We believe this drug may be the reason, but we need to study more patients to make sure."
The researchers will begin a larger study in the next few weeks. Lenze, the director of the Healthy Mind Lab at the School of Medicine, is an expert in using mobile and internet technology to conduct clinical trials. He said that although this initial study involved patients in the St. Louis region, the next phase of the research will involve patients from throughout the country.
"We bring the study to the patients, giving them tools to monitor their health at home," Lenze said. "Our hope is that we can keep these patients healthy enough to avoid hospitalization."
This work was supported by the Taylor Family Institute for Innovative Psychiatric Research, the Bantly Foundation, the Center for Brain Research in Mood Disorders at Washington University and the COVID-19 Early Treatment Fund. Additional support from the National Center for Advancing Translational Sciences of the National Institutes of Health (NIH). Grant number UL1 TR002345.
Tuesday, April 6, 2021
Newly discovered antibiotics kill bacteria differently
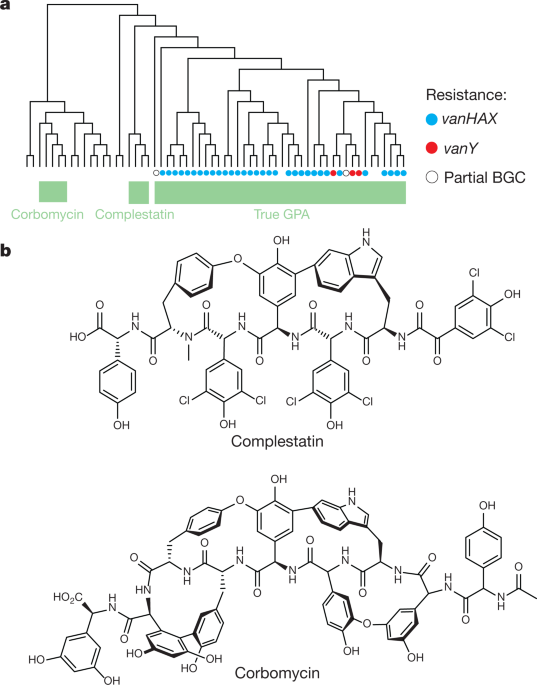
'Holy grail' of antibiotics
Unique bacteria killer
Fight against antibiotic resistance
Monday, May 31, 2010
Plectasin - a new weapon against highly resistant microbes ?..
In this process, plectasin behaves like a thief which steals the stones off a mason. 'It binds to a cell-wall building block called lipid II and thus prevents it from being incorporated ,' Professor Sahl explains. 'However, bacteria cannot live without a cell wall.' It comes as no surprise that the most famous antibiotic penicillin also inhibits cell-wall synthesis...
Tuesday, May 26, 2009
Aerosol delivery of antibiotics via nanoparticles !
Treatment with antibiotic-laden nanoparticles effectively eliminated respiratory infections in mice that had been inoculated with Pseudomona aeroginosa, a common bacterial species that often infects the respiratory tract in humans, particularly immunocompromised patients, ventilated patients or those with cystic fibrosis. Infected mice that inhaled aerosolized nanoparticles encapsulating silver carbene complexes (SCCs), a novel class of silver-based antimicrobials with broad-spectrum activity, showed a significant survival advantage over the control mice that received nanoparticles without the SCCs. The results are really interesting and even the half the dose is sufficient. Toxicity results are still to be done, however this is a good beginning and hope they will come up with interesting results in the near future...
Ref :http://www.thoracic.org/sections/publications/press-releases/conference/articles/2009/abstracts-and-press-releases/cannon.pdf
Saturday, November 23, 2013
Ticagrelor drug may reduce risk of dying following heart attack
"Adenosine has many different effects in the body including influencing the activity of white blood cells that are involved in tackling pneumonia and other infections."
Thursday, May 19, 2016
Novartis announces FDA approval of Afinitor for progressive, nonfunctional neuroendocrine tumors of GI

Monday, December 25, 2017
Benzodiazepines linked to increased risk of death among Alzheimer’s disease patients
Monday, December 4, 2017
FDA Approves Alecensa (alectinib) as First-Line Treatment for ALK-Positive Metastatic Non-Small Cell Lung Cancer
“Our goal is to develop medicines that have the potential to significantly improve upon the standard of care,” said Sandra Horning, M.D., chief medical officer and head of Global Product Development. “In our pivotal study, Alecensa significantly extended the time that people lived without their disease worsening compared to crizotinib and also showed a marked reduction in the risk of their cancer spreading to the brain.”
“ALK-positive lung cancer is often found in younger people, who tend to have more advanced disease at the time of diagnosis, and comes with a unique set of challenges," said Bonnie J. Addario, a lung cancer survivor and founder of the Bonnie J. Addario Lung Cancer Foundation (ALCF). “We applaud advancements in care, like the approval of Alecensa, which provides a new initial treatment option for people with this type of lung cancer.”
Thursday, July 12, 2018
Drug to treat bleeding may benefit some stroke patients, study finds
Nikola Sprigg, Professor of Stroke Medicine at the Stroke Trials Unit in the University's Division of Clinical Neuroscience, led the trial. She said: "Tranexamic acid is cheap—costing less than £15 per patient—and widely available so has the potential for reducing death and disability across the world."
"While we failed to show significant benefits three months after stroke, the reduction in early deaths, amount of bleeding on the brain and serious complications are signs that this drug may be of benefit in the future. More trials are needed, particularly focusing on giving treatment as soon as possible after the start of bleeding in this emergency condition."TICH-2 cements the position of the NIHR and the UK as key players in the world of stroke research. A study of this scale would simply not have been possible without support of the NIHR infrastructure. Alongside the large stroke centres, the contribution made by the network of smaller sites across the UK has been crucial to the success of TICH-2."
Thursday, July 24, 2014
Zydelig Approved for Three Types of Blood Cancer
Thursday, December 1, 2016
Theravance Biopharma Announces FDA Approval of Expanded Label for Vibativ (telavancin)

Expanded Vibativ Label Data
- In the all-treated cSSSI patient population with baseline S. aureus bacteremia in the ATLAS I and II trials, clinical cure rates at test-of-cure were 57.1% for Vibativ-treated patients vs. 54.6% for vancomycin-treated patients.
- In the HABP/VABP patient population with at least one Gram-positive respiratory pathogen at baseline who had concurrent S. aureus bacteremia in the ATTAIN I and II trials, the 28-day all-cause mortality rate was 40.0% for Vibativ-treated patients vs. 39.5% for vancomycin-treated patients.




