Tuesday, December 16, 2025
FDA Grants Accelerated Approval to Hernexeos (zongertinib) for Previously Treated Patients with HER2-Mutant Advanced NSCLC
Wednesday, August 13, 2025
FDA Approves Arynta (lisdexamfetamine) Oral Solution for ADHD and Binge Eating Disorder
Tuesday, August 12, 2025
FDA Approves Harliku (nitisinone) for the Treatment of Patients with Alkaptonuria
Friday, July 25, 2025
FDA Approves Ibtrozi (taletrectinib) for Advanced ROS1-Positive Non-Small Cell Lung Cancer
Nuvation Bio Inc. announced the U.S. Food and Drug Administration (FDA) approval of Ibtrozi (taletrectinib) for the treatment of adult patients with locally advanced or metastatic ROS1-positive (ROS1+) non-small cell lung cancer (NSCLC). Ibtrozi is a highly selective, next-generation oral ROS1 tyrosine kinase inhibitor (TKI) designed to address some of the outstanding challenges of treating ROS1+ NSCLC. It has demonstrated high response rates with durable benefit and intracranial activity and is generally well tolerated, providing a new treatment option for patients with advanced ROS1+ NSCLC.
“The FDA approval of Ibtrozi marks a major milestone in the evolution of targeted therapy for advanced ROS1-positive NSCLC,” said David Hung, M.D., Founder, President and Chief Executive Officer of Nuvation Bio. “We believe one of the greatest threats to ROS1-positive lung cancer patients is disease progression, especially in the first-line setting. In pivotal trials, Ibtrozi delivered high response rates with sustained durability—truly meaningful benefits for patients. With its clinically proven efficacy and safety profile, we believe Ibtrozi has the potential to become a new standard for what targeted therapies can achieve in this type of lung cancer. With approvals for Ibtrozi now in the U.S. and China, and additional global filings underway, we remain committed to delivering innovative therapies that help patients stay ahead of their disease.”
ROS1+ NSCLC is a rare and aggressive form of lung cancer, accounting for approximately 2% of new NSCLC cases, or about 3,000 new diagnoses of advanced disease annually in the U.S. The median age at diagnosis for patients with this type of lung cancer is approximately 50 years old, and the disease is more likely to occur in people who have never smoked. Brain metastases are common and a leading cause of disease progression and mortality in this population.
“For people living with advanced ROS1-positive lung cancer, who tend to be diagnosed at a younger age, having another treatment option can make a real difference for them and their loved ones,” said Janet Freeman-Daily, Co-Founder and President of The ROS1ders. “The approval of this new targeted therapy is a meaningful step forward for the advanced ROS1+ lung cancer community and offers hope for patients facing the added challenge of cancer spreading to the brain.”
The FDA approval of Ibtrozi is supported by one of the largest global clinical trial programs in ROS1+ NSCLC to date, with over 300 patients enrolled in the pivotal TRUST-I and TRUST-II studies.
In TRUST-I, Ibtrozi achieved a confirmed overall response rate (cORR) of 90% in TKI-naïve patients. These findings were reinforced by the TRUST-II results, with a cORR of 85% in TKI-naïve patients. The median duration of response (DOR) was not yet reached for either trial, based on a cutoff date that is nearly five months later than that of the pooled TRUST-I and TRUST-II analysis published in April in the Journal of Clinical Oncology. For TRUST-I, with a median follow-up for responses of 40 months, the longest DOR was observed at 46.9 months and ongoing. For TRUST-II, with a median follow-up for responses of 19 months, the longest DOR was observed at 30.4 months and ongoing as of October 2024. Given the single-arm nature of the TRUST clinical studies, median progression-free survival (PFS) is not provided in the label.
Across the pivotal studies, consistent results were also observed among patients who were previously treated with a ROS1 TKI (TKI-pretreated). In TRUST-I, treatment with Ibtrozi achieved a cORR of 52% and median DOR of 13.2 months for TKI-pretreated patients, with median follow-up for responses of 33 months. In TRUST-II, treatment with Ibtrozi achieved a cORR of 62%, and as of October 2024 the median DOR was 19.4 months in these patients, with a median follow-up for responses of 19 months.
Brain metastases are among the most common and devastating complications in advanced ROS1+ NSCLC. Ibtrozi was designed to penetrate the central nervous system (CNS) and has demonstrated consistent intracranial responses in patients with measurable brain metastases at baseline. An intracranial response was achieved in 73% of TKI-naive patients (11/15) and 63% of TKI-pretreated patients (15/24).
“Patients living with advanced ROS1+ non-small cell lung cancer and their healthcare providers are in need of new treatment options,” added Nathan Pennell, M.D., Ph.D., TRUST study investigator and Professor of Medicine at the Cleveland Clinic. “Ibtrozi’s durability of response and ability to effectively penetrate the brain, coupled with a well-characterized and manageable safety profile, further addresses these critical needs for patients. I believe this now-approved therapy offers providers and patients a promising new option for the treatment of advanced ROS1+ non-small cell lung cancer.” Dr. Pennell is a compensated member of Nuvation Bio’s advisory committee.
Ibtrozi was generally well-tolerated, with most adverse events being low grade, transient and manageable. Patients infrequently (7%) discontinued treatment due to treatment-emergent adverse events (TEAEs). The most common adverse reactions (≥20%) included diarrhea (64%), nausea (47%), vomiting (43%), dizziness (22%), rash (22%), constipation (21%), and fatigue (20%). Overall, the majority of CNS events were mild to moderate (~90%) and resolved within days, and dose modifications due to these events were low (~5%). Approximately 90% of reported cases of dizziness were Grade 1 (mild) and transient. Liver enzyme elevations (AST 87%/ALT 85%) and QT prolongation (19%) were manageable with standard monitoring and dose modifications. Ibtrozi is approved as a 600 mg once-daily oral dose, supported by a half-life of approximately 66 hours and broad tissue distribution, including the brain, enabling sustained systemic and CNS exposure.
Saturday, June 14, 2025
FDA Approves Mezofy (aripiprazole) Oral Film for the Treatment of Schizophrenia
In continuation of my update on Aripiprazole
CMG Pharmaceuticals, an affiliate of Cha Biotech, announced on the 16th that it had received product approval for the schizophrenia treatment drug Mezofy (formerly Depibzo) from the U.S. Food and Drug Administration (FDA).
Mezofy is an oral film-type schizophrenia treatment drug (ingredient name: aripiprazole) developed by CMG Pharmaceuticals. Patients with mental illnesses including schizophrenia often refuse or spit out medication, but the film-type drug can be taken without water and easily dissolves in the mouth, solving this problem.
CMG Pharmaceuticals first applied for FDA approval in December 2019. At that time, CMG Pharmaceuticals was the world’s first film-type schizophrenia treatment company to knock on the FDA’s door. However, the supplementary inspection was delayed due to problems with overseas raw material factories and the impact of the COVID-19 pandemic.
Meanwhile, Opipza, aripiprazole film treatment from China's LP Pharma, received FDA approval in July of last year. CMG Pharmaceuticals then reapplied for product approval in October of last year and received marketing approval.
Mezofy is the fourth product from a domestic pharmaceutical company to receive FDA approval for an improved new drug. An improved new drug is not simply a copy of a new drug whose patent has expired, but rather an improvement in the dosage method by changing the efficacy or formulation. Unlike simple generic drugs, it is protected separately by a patent.
The company explained, “The price of improved new drugs is set higher than that of generic drugs, and they can be marketed and prescribed under the product name rather than the ingredient name, which is advantageous in increasing awareness in the market.”
The company predicted that the market for Mezofy would expand to over KRW 22 trillion when its indications are expanded to include bipolar disorder, major depressive disorder, autism spectrum disorder, and Tourette's disorder.
The company said, “We plan to complete the selection of a local distribution partner in the U.S. by the second half of this year,” and “We will work with our distribution partners to establish a competitive drug pricing strategy.”
CMG Pharmaceuticals has set a goal of achieving annual sales of over 100 billion won within five years of entering the U.S. market. CMG Pharmaceuticals CEO Lee Ju-hyung said, “After proving the excellence of Mezofy in the U.S. market, we will advance into other overseas markets.”
At the time of the initial application for product approval, the product name was Depipzo. The company explained that in collaboration with the global pharmaceutical branding specialist Brand Institute, it decided on Mezofy as a name that is easier to remember and less likely to cause prescription errors.
Thursday, June 12, 2025
FDA Approves Atzumi (dihydroergotamine) Nasal Powder for the Acute Treatment of Migraine
Monday, January 24, 2022
FDA Approves Apretude
Cabotegravir long-acting for PrEP is provided as an injection given as few as six times per year and is initiated with a single 600 mg (3-ml) injection given one month apart for two consecutive months. After the second initiation injection, the recommended continuation injection dose is a single 600 mg (3-ml) injection given every two months. Vocabria (cabotegravir oral tablets) may be administered for approximately one month before initiating the first injection to assess the tolerability of the medicine.
Deborah Waterhouse, CEO, ViiV Healthcare, said: “People who are vulnerable to acquiring HIV, especially those in Black and Latinx communities who are disproportionately impacted in the US, may want options beyond daily oral pills. That’s why ViiV Healthcare is proud that Apretude was studied in one of the most diverse and comprehensive HIV prevention trial programs to date, which also included some of the largest numbers of transgender women and Black men who have sex with men ever enrolled in an HIV prevention trial. With Apretude, people can reduce the risk of acquiring HIV with as few as six injections a year. Today’s approval is the latest example of ViiV Healthcare’s commitment to developing long-acting medicines that offer consumers a different choice.”
US FDA approval is based on the results from two international phase IIb/III multicenter, randomised, double-blind, active-controlled trials, HPTN 083 and HPTN 084, which evaluated the safety and efficacy of cabotegravir long-acting for PrEP in HIV-negative men who have sex with men, transgender women, and cisgender women, who were at increased risk of sexually acquiring HIV. In these trials, which included more than 7,700 participants across 13 countries combined, the blinded, randomised portions of both trials were stopped early by an independent Data Safety Monitoring Board after cabotegravir long-acting for PrEP was shown to be superior to daily oral emtricitabine/tenofovir disoproxil fumarate (TDF/FTC) tablets in preventing the acquisition of HIV in study participants. Clinical trial participants who received cabotegravir long-acting for PrEP experienced a 69% lower incidence of HIV compared to FTC/TDF tablets in HPTN 083 and a 90% lower incidence of HIV compared to FTC/TDF tablets in HPTN 084.
The most common adverse reactions (all grades) observed in at least 1% of clinical trial participants receiving cabotegravir long-acting for PrEP were injection site reactions, diarrhoea, headache, pyrexia, fatigue, sleep disorders, nausea, dizziness, flatulence, abdominal pain, vomiting, myalgia, rash, decreased appetite, somnolence, back pain, and upper respiratory tract infection. Adverse events led to discontinuation in 6% of participants in HPTN 083 and 1% of participants in HPTN 084.
In HPTN 083, participants in the US were inclusive of the Black/African American and Latinx communities of men and transgender women who have sex with men, who are disproportionately affected by the HIV epidemic and comprise the greatest percentage of new HIV diagnoses. In HPTN 084, all participants were cisgender women from sub-Saharan Africa. Women in this region bear a disproportionate burden of the HIV epidemic and may be twice as likely to acquire HIV as their male counterparts.
Richard Elion, MD, Director of Research at Washington Health Institute, said: “We have the tools to end the HIV epidemic through the implementation of effective antiretroviral treatment and HIV prevention. PrEP has played a vital role in protecting people from acquiring HIV. With the availability of cabotegravir long-acting for PrEP as an injection every two months to prevent HIV, people now have an important new option besides daily medication. This long-acting medication offers more options for prevention, and now providers and patients will be empowered by choices and the ability to choose the approach that is optimal for each individual.”
HIV continues to be a global public health crisis, with an estimated 38 million people living with HIV worldwide and 1.7 million new cases annually. PrEP represents an effective tool to reduce new cases of HIV, which in addition to successful HIV antiretroviral treatment, will help efforts to end the HIV epidemic. However, fewer than 25% of the people who could benefit from PrEP in the US are currently taking it. Despite the wide availability of daily oral PrEP, it can be limited by inconsistent adherence as well as structural and cultural barriers that lead to underutilisation in key populations.
https://www.drugs.com/apretude.html
https://www.drugs.com/newdrugs/fda-approves-apretude-cabotegravir-extended-release-injectable-suspension-hiv-pre-exposure-5754.html
Thursday, November 19, 2020
FDA Approves Zeposia (ozanimod) for Relapsing Forms of Multiple Sclerosis

- Zeposia demonstrated a relative reduction in ARR versus AVONEX of 48% through one year and 38% at two years (absolute ARR of 0.18 versus 0.35 and 0.17 versus 0.28, respectively).1,2,3
- At one year, treatment with Zeposia reduced the number of T1-weighted gadolinium-enhanced (GdE) brain lesions more than AVONEX (0.16 vs 0.43), a relative reduction of 63%, and reduced the number of new or enlarging T2 lesions (1.47 vs. 2.84), a relative reduction of 48%.1,3
- At two years, treatment with Zeposia reduced the number of T1-weighted gadolinium-enhanced (GdE) brain lesions more than AVONEX (0.18 vs 0.37), a relative reduction of 53%.1,2 Zeposia also reduced the number of new or enlarging T2 lesions vs AVONEX (1.84 vs 3.18), a relative reduction of 42%.1,2
FDA Approves Zeposia (ozanimod) for Relapsing Forms of Multiple Sclerosis
Friday, November 13, 2020
FDA Approves Isturisa (osilodrostat) for the Treatment of Cushing’s Disease
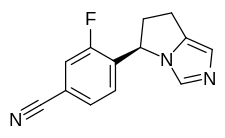
“The FDA supports the development of safe and effective treatments for rare diseases, and this new therapy can help people with Cushing’s disease, a rare condition where excessive cortisol production puts them at risk for other medical issues,” said Mary Thanh Hai, M.D., acting director of the Office of Drug Evaluation II in the FDA’s Center for Drug Evaluation and Research. “By helping patients achieve normal cortisol levels, this medication is an important treatment option for adults with Cushing’s disease.”
------------------------------------------------------------------------------------------------------------------
FDA Approves Isturisa (osilodrostat) for the Treatment of Cushing’s Disease
Tuesday, December 24, 2019
Ipsen Announces U.S. FDA Approval for Newly Designed Pre-Filled Syringe for Somatuline Depot (lanreotide)

“The conditions of GEP-NETs and acromegaly can be associated with a number of uncomfortable and unpleasant symptoms, and innovation aimed at improving the injection process is a step forward,” said Daphne Adelman, Clinical Nurse Specialist, Northwestern University, Chicago, and one of the authors of the study.
“We consistently look for opportunities to respond to the needs of the communities we serve, and this approval would not have been possible without the direct involvement of nurses and the patients with GEP-NETs and acromegaly whom they treat,” said Bradley Bailey, SVP, and Franchise Head Oncology/Endocrinology Business Unit at Ipsen. “We listened and collaborated to enhance the existing pre-filled syringe, making it sturdier for healthcare providers when administering treatment, with the intention of improving the injection process. We look forward to bringing this innovation to healthcare providers for their patients soon.”
Wednesday, July 3, 2019
FDA Approves Mavyret (glecaprevir and pibrentasvir) as First Treatment for All Genotypes of Hepatitis C in Pediatric Patients
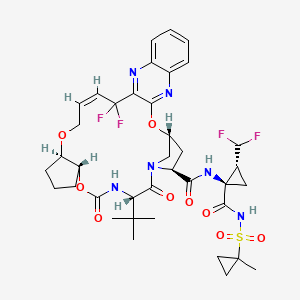
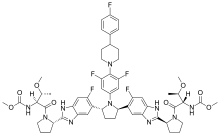 Pibrentasvir
Pibrentasvir“Direct-acting antiviral drugs reduce the amount of HCV in the body by preventing the virus from multiplying, and in most cases, they cure HCV infection,” said Jeffrey Murray, M.D., M.P.H., deputy director of the Division of Antiviral Products in the FDA’s Center for Drug Evaluation and Research. “Today’s approval represents another treatment option for children and adolescents with HCV infection, but for the first time, in all genotypes of HCV.”
Tuesday, July 2, 2019
FDA Approves Qternmet XR (dapagliflozin, saxagliptin and metformin hydrochloride) for Type 2 Diabetes

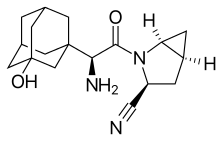 Saxagliptin and
Saxagliptin and About Qternmet XR
Saturday, April 27, 2019
FDA Approves Jatenzo (testosterone undecanoate) for Certain Forms of Hypogonadism








