Wednesday, March 31, 2021
Statin use alone or with metformin may increase survival in high-risk prostate cancer patients
Friday, January 29, 2021
Statins May Protect Heart From Chemo for Early Breast Cancer
For women with early breast cancer treated with anthracyclines, statin exposure is associated with a lower risk for hospital presentation for heart failure, according to a study published online Jan. 6 in the Journal of the American Heart Association.
Husam Abdel-Qadir, M.D., Ph.D., from the Women's College Hospital in Toronto, and colleagues conducted a retrospective cohort study involving women aged 66 years and older without prior heart failure who received anthracyclines or trastuzumab for newly diagnosed early breast cancer. Using propensity scores, statin-exposed and unexposed women were matched in a 1:1 ratio. Data were included for 666 statin-discordant pairs of anthracycline-treated women and 390 pairs of trastuzumab-treated women.
The researchers found that the five-year cumulative incidence of heart failure hospital presentations after anthracyclines was 1.2 percent (95 percent confidence interval [CI], 0.5 to 2.6 percent) and 2.9 percent (95 percent CI, 1.7 to 4.6 percent) in statin-exposed and unexposed women, respectively (P = 0.01). In the anthracycline cohort, the cause-specific hazard ratio associated with statins was 0.45 (95 percent CI, 0.24 to 0.85; P = 0.01). The five-year cumulative incidence of heart failure hospital presentations after trastuzumab was 2.7 percent (95 percent CI, 1.2 to 5.2 percent) and 3.7 percent (95 percent CI, 2.0 to 6.2 percent) in statin-exposed and unexposed women, respectively (P = 0.09), with a cause-specific hazard ratio associated with statins of 0.46 (95 percent CI, 0.20 to 1.07; P = 0.07).
"This study does not conclusively prove statins are protective," Abdel-Qadir said in a statement. "However, this study builds on the body of evidence suggesting that they may have benefits."
Wednesday, January 13, 2021
AHA: Adding Omega-3 Fatty Acids Does Not Cut High CV Risk
In continuation of my update on omega-3 fatty acids
A carboxylic acid formulation of eicosapentaenoic acid and docosahexaenoic acid (omega-3 CA) does not improve outcomes among statin-treated patients at high cardiovascular risk, according to a study published online Nov. 15 in the Journal of the American Medical Association to coincide with the American Heart Association Scientific Sessions 2020, held virtually from Nov. 13 to 17.
Stephen J. Nicholls, M.B.B.S., Ph.D., from Monash University in Melbourne, Australia, and colleagues conducted a double-blind trial comparing omega-3 CA to corn oil in 13,078 statin-treated patients with high cardiovascular risk, hypertriglyceridemia, and low high-density lipoprotein cholesterol from 675 academic and community hospitals in 22 countries. Participants were randomly assigned in a 1:1 ratio to either 4 g/day omega-3 CA or corn oil (6,539 to each) in addition to usual background therapies, including statins.
"These findings do not support use of this omega-3 fatty acid formulation to reduce major adverse cardiovascular events in high-risk patients," the authors write.
Several authors disclosed financial ties to pharmaceutical companies, including AstraZeneca, which funded the study.
Thursday, April 9, 2020
Aspirin May No Longer Have Effect in Primary CVD Prevention
"In a modern era characterized by widespread statin use and population-wide cancer screening, aspirin no longer reduces the absolute risk of cancer death or myocardial infarction when given as primary prevention," the authors write.
Saturday, July 6, 2019
Statin Use Associated With Higher Incidence of Diabetes
"As lifestyle programs like the Diabetes Prevention Program are promoted in primary care settings, we hope physicians will integrate and insurers support healthy lifestyle strategies as part of the optimal management of individuals at risk for both new-onset diabetes and cardiovascular disease," the authors write.
Thursday, March 14, 2019
Statins Help the Heart, No Matter What Your Age
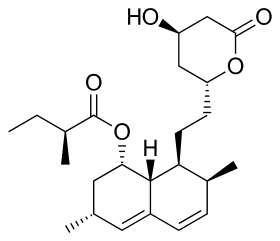
Cholesterol-lowering statins are already known to help cut heart risks for seniors and the middle-aged. Now, research confirms the meds can also help people aged 75 and older.
"Statin therapy has been shown to prevent cardiovascular disease in a wide range of people, but there has been uncertainty about its efficacy and safety among older people," said lead investigator Anthony Keech. He's a professor of medicine, cardiology and epidemiology at the University of Sydney in Australia.
"Our study summarized all the available evidence from major trials to help clarify this issue. We found that there were significant reductions in major vascular events in each of the six age groups considered, including patients [who were] aged over 75 at the start of treatment," Keech said in an Oxford news release.
"Statin therapy appears to be just as effective in people aged over 75 years as it is in younger people," study co-investigator Jordan Fulcher said in the news release. Fulcher is a cardiovascular research fellow at the University of Sydney.
"We have definitive evidence that statins benefit older people who have suffered a heart attack or stroke. Fewer healthy older people were represented in these trials, so more information in this group of people would help confirm the same benefits that we see in our overall trials population," he said.
"Since the risk of heart attack and stroke increases with age, the potential benefits are likely to be even greater for older people," he said.
"Therefore, there is a need to ensure that patients at risk of cardiovascular disease due to their age are offered statin therapy where there is good reason to believe that it will be beneficial," Baigent said.
Wednesday, September 20, 2017
Two anticlotting medicines better at reducing bleeding risk than triple therapy
 rivaroxaban
rivaroxaban 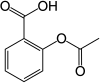 Aspirin
AspirinThursday, September 14, 2017
Fenofibrate drug may reduce risk of cardiovascular events in patients with type 2 diabetes

Friday, April 14, 2017
New research shows how cholesterol medicine has beneficial effect on immune defence system
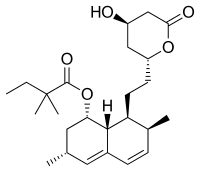
Monday, October 24, 2016
Statins may shield unborn babies from mother's stress, study suggests
Tuesday, October 18, 2016
High fruit intake during adolescence linked with lower breast cancer risk: But increasing alcohol intake in later life associated with higher risk

Friday, June 17, 2016
Evolocumab could be more effective than ezetimibe in lowering cholesterol in statin-intolerant patients

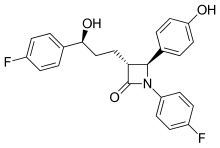
- In Phase A, patients were assigned to two groups. Each group was treated for 10 weeks with atorvastatin or placebo in a blinded fashion, then crossed over to the alternate therapy for another 10 weeks. Patients were asked to report any muscle pain or weakness.
- Patients who reported intolerable muscle symptoms on atorvastatin, but not placebo, moved to Phase B. In this 24-week phase, patients with confirmed statin intolerance were administered two alternative non-statin therapies, ezetimibe vs. evolocumab.
- The research is being presented at the American College of Cardiology's 65th Annual Scientific Session and simultaneously published online in the Journal of the American Medical Association."Statin intolerance has been a very challenging clinical problem," said Steven Nissen, M.D., chairman of Cardiovascular Medicine at Cleveland Clinic. "The study showed that PCSK9 inhibitors can significantly lower cholesterol in patients with documented statin intolerance, providing an effective treatment for these difficult to manage patients."The GAUSS-3 trial enrolled 511 patients with very high levels of LDL cholesterol - averaging more than 210 mg/dL ¬¬- and with a history of muscle-related statin intolerance. More than 80% of participants had previously reported intolerance to three or more statins. The study showed that 42.6 percent of these patients reported muscle pain or weakness on atorvastatin, but not placebo, and 26.5 percent on the placebo, but not atorvastatin.
Friday, August 14, 2015
Cholesterol-lowering statin drugs could delay prostate cancer growth in patients receiving ADT
Tuesday, January 6, 2015
Cholesterol Drug Vytorin Linked to Reduced Heart Attack Risk
Thursday, December 11, 2014
Cholesterol-fighting statins inhibit uterine fibroid tumors that account for 50% of hysterectomies...
Sunday, September 28, 2014
Rosuvastatin promotes bone growth in mice with achondroplasia symptoms
Friday, April 11, 2014
Statins could ease coughing in lung disease patients, study finds -- ScienceDaily
Friday, November 1, 2013
New Cholesterol-Lowering Drug, ALN-PCS Shows Early Promise
"Cardiovascular disease remains the leading cause of death of men and women globally and reduction of LDL cholesterol with statin medications has been demonstrated to substantially reduce the risk of first or recurrent cardiovascular events," said Dr. Gregg Fonarow, a professor of cardiology at the University of California, Los Angeles.
Sunday, January 6, 2013
Common cholesterol-lowering drug may help protect against cerebral malaria
"The molecular mechanisms that give rise to cerebral malaria and subsequent cognitive dysfunction are not yet known," says Zimmerman. "However, the fact that statin treatment decreases both injurious blood vessel inflammation and cognitive dysfunction suggests that a combination of vascular and inflammatory triggers leads to cerebral pathology and intellectual deficits."Ref : http://www.plospathogens.org/article/info%3Adoi%2F10.1371%2Fjournal.ppat.1003099
Common cholesterol-lowering drug may help protect against cerebral malaria
Friday, November 9, 2012
New medication lomitapide, shows promise as lipid-lowering therapy for rare cholesterol disorder
"The magnitude of this reduction in LDL-C and the fact that some patients reached or approached the LDL-C therapeutic goals is truly remarkable for this high risk population that historically doesn't respond to lipid-lowering drugs," said the study's lead author, Marina Cuchel, MD, PhD, research assistant professor of Medicine at Penn. "A reduction in LDL-C of this magnitude is certainly expected to favorably alter the clinical course of this devastating disease."


