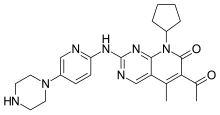
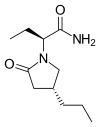
In continuation of my update on Ibrutinib
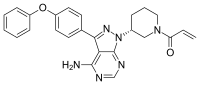
AbbVie (NYSE: ABBV), a global biopharmaceutical company, today announced the U.S. Food and Drug Administration (FDA) approved Imbruvica (ibrutinib) as a first-line treatment for patients with chronic lymphocytic leukemia (CLL).1 The approval is based on data from the randomized, multi-center, open-label Phase 3 RESONATE™-2 (PCYC-1115) trial, which evaluated the use of Imbruvica versus chlorambucil in 269 treatment-naïve patients with CLL or small lymphocytic lymphoma (SLL) aged 65 years or older. The RESONATE-2 data were previously presented at the American Society of Hematology (ASH) Annual Meeting in December 2015 and also simultaneously published in The New England Journal of Medicine. Imbruvica is jointly developed and commercialized by Pharmacyclics LLC, an AbbVie company and Janssen Biotech, Inc.
"This approval represents a significant leap forward for patients diagnosed with CLL who may want to consider an alternative first-line treatment to traditional chemotherapy," said Michael Severino, M.D., executive vice president, research and development and chief scientific officer, AbbVie. "AbbVie is committed to making significant improvements in the lives of patients with hematologic malignancies and will continue to explore ways to improve treatment options for patients."
The prevalence of CLL is approximately 115,000 patients in the U.S.2 with approximately 15,000 newly diagnosed patients every year.3 CLL is a disease of elderly patients, with an average diagnosis age of 71.3
The National Comprehensive Cancer Network (NCCN) recently published an update to its clinical practice guidelines for non-Hodgkin's lymphomas, granting Imbruvica a category 1 recommendation for certain CLL patients, the highest recommendation assigned by the organization. Specifically, NCCN recommends Imbruvica as a first-line treatment option for frail CLL patients with significant comorbidities, as well as for CLL patients with or without del 17p or the genetic mutation TP53 who are 70 years or older, or younger patients with significant comorbidities. The NCCN guidelines inform prescribing and reimbursement practices in many institutions in the U.S. and internationally.
"The progression-free survival data seen in these previously untreated CLL patients are strong and encouraging," said Dr. Jan Burger, M.D., Ph.D., Associate Professor, Department of Leukemia, Division of Cancer Medicine, The University of Texas MD Anderson Cancer Center, Houston, TX and the RESONATE-2 lead study investigator.* "This is especially important for first-line CLL patients, when considering the safety profile. This treatment represents another option for these patients."
FDA Approves Imbruvica (ibrutinib) for the First-Line Treatment of Chronic Lymphocytic Leukemia


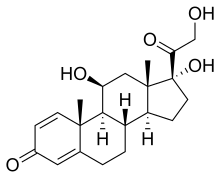 (Prednisole)
(Prednisole) (Indomethacin)
(Indomethacin)