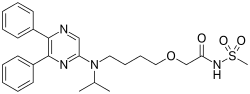
In continuation of my update on Selexipag
Selexipag (trade name: Uptravi) is approved for long-term treatment of pulmonary arterial hypertension (PAH) in adults with moderate to severe symptoms. The drug can be used either as combination therapy with other blood-pressure lowering drugs or as monotherapy in patients who are not candidates for these therapies. Selexipag has been on the market in Germany since May 2016. In an early benefit assessment, the German Institute for Quality and Efficiency in Health Care (IQWiG) has now examined whether this drug has advantages or disadvantages in comparison with the appropriate comparator therapy.
The limitation of the comparator therapy to a specific drug and the subsequent division of the population in the dossier were inadequate. The only study cited by the drug manufacturer for one of its subpopulations compared selexipag with placebo. However, no added benefit can be inferred from such a comparison.
Hence the manufacturer presented no suitable data for the assessment of the added benefit of selexipag, and IQWiG concluded: An added benefit of selexipag in comparison with the appropriate comparator therapy is not proven.
Selective widening of vessels and inhibition of tissue growth
In PAH, the pulmonary artery is narrowed, and the heart has to work harder to pump oxygen-poor blood through the pulmonary artery into the lungs. The permanently increased workload of the right heart chamber decreases the body's oxygen supply. The high blood pressure (hypertension) is often caused by another heart or lung disease, e.g. by chronic obstructive pulmonary disease (COPD) or a congenital heart defect.
Selexipag aims to widen the pulmonary artery and slow down the overload of the heart. The drug is approved for long-term treatment of PAH patients who have no symptoms at rest but who have slight (WHO functional class II) or marked (WHO functional class III) limitation of physical activity. These restrictions cause symptoms such as dyspnoea, tiredness, chest pain, or dizziness. Selexipag is an option as combination therapy in patients insufficiently controlled with an endothelin receptor antagonist (ERA) and/or a phosphodiesterase-5 (PDE-5) inhibitor, or as monotherapy in patients who are not candidates for these therapies.





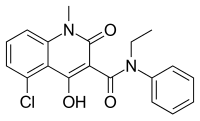

 Midostaurin
Midostaurin